Neurological physical therapy includes everything from head injuries and stroke rehabilitation to cerebral palsy and multiple sclerosis. Regardless of the condition you're dealing with, some general things hold true for all patients seeking treatment. Let's take a closer look at what those are in this comprehensive guide.
The plasticity of the brain was once believed to be limited, but recent research has revealed its remarkable ability to adapt. Physical therapy utilizes specific exercises and techniques that stimulate the brain's ability to create new neural connections, reorganize existing ones, and adapt to changes in the body.1
By harnessing the brain's plasticity, physical therapy can help individuals recover from injury or illness, improve their physical abilities, and maintain optimal health and function over time.
In this article, we will focus on how neurological physical therapy can help address brain and spinal cord dysfunction, also known as the central nervous system (CNS).
Table of Contents
- Understanding the Brain and Head
- What is a Focal Neurological Deficit?
- What is a Non-Focal Neurological Deficit?
- Common Causes of Brain Dysfunction
- Other Head Dysfunction
- How a Neurological Physical Therapist Can Help
- What to Expect from Your Physical Therapist
- Is Virtual Physical Therapy Appropriate for a Head, Spinal Cord, or Brain Injury?
- How to Optimize Your Brain and Spinal Cord Health
- Getting the Care You Need: Is It Time?
Understanding the Brain and Head
To understand how neurological physical therapy can help patients with neurological deficits, it's important first to understand a little bit about the brain (and head) and how it works.
The brain is made up of billions of cells called neurons, which send and receive electrical signals. These signals allow us to think, feel, and move. The brain is also divided into different regions, each responsible for specific functions.
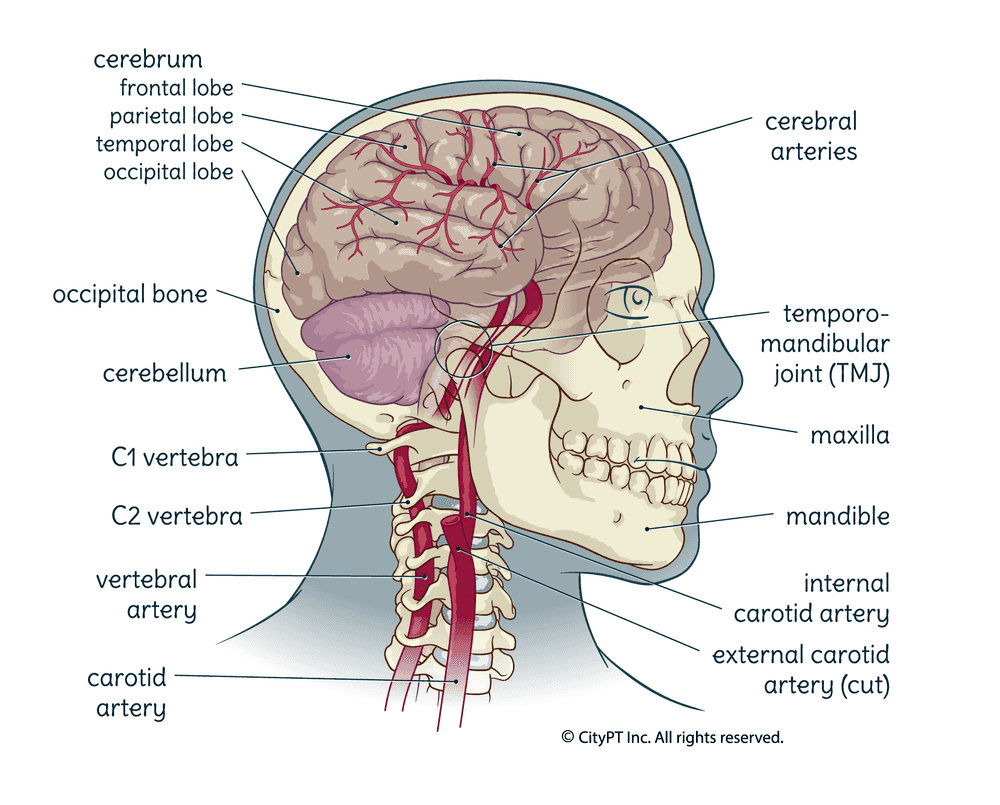
Let's review the basic regions of the central nervous system:2
- Cerebrum: This is the largest region of the brain and is responsible for our higher-level functions, such as reasoning, problem-solving, and planning. It includes:
- The frontal lobe, which controls things like movement and decision-making
- The temporal lobes (sides), responsible for memory and hearing
- The parietal lobe (top middle), which helps us process information about touch, taste, and movement
- The occipital lobe (base of the brain), responsible for interpreting vision
- Cerebellum: This region is located under the cerebrum and helps with balance, coordination, and muscle movement.
- Brainstem: This region connects the brain to the spinal cord and controls basic functions like breathing and heart rate.
Other Key Areas of the Brain that Help The Body Thrive
- Pineal gland: This small gland is located near the center of the brain and helps to regulate our sleep-wake cycles.
- Pituitary gland: This gland is located at the base of the brain and produces hormones that help us grow, reproduce, and maintain our metabolism.
- Hypothalamus: This area of the brain helps to regulate things like hunger, thirst, body temperature, and blood pressure.
- Amygdala: This almond-shaped region is responsible for our emotions, including fear and aggression.
- Hippocampus: This region helps us form new memories and is essential for learning and recall.
- Basal ganglia: This area of the brain is involved in motor control and coordination.
- Cranial nerves: These are a set of 12 nerves that originate in the brain and provide sensation to the head and face, as well as control movement of the face, neck, and other muscles.
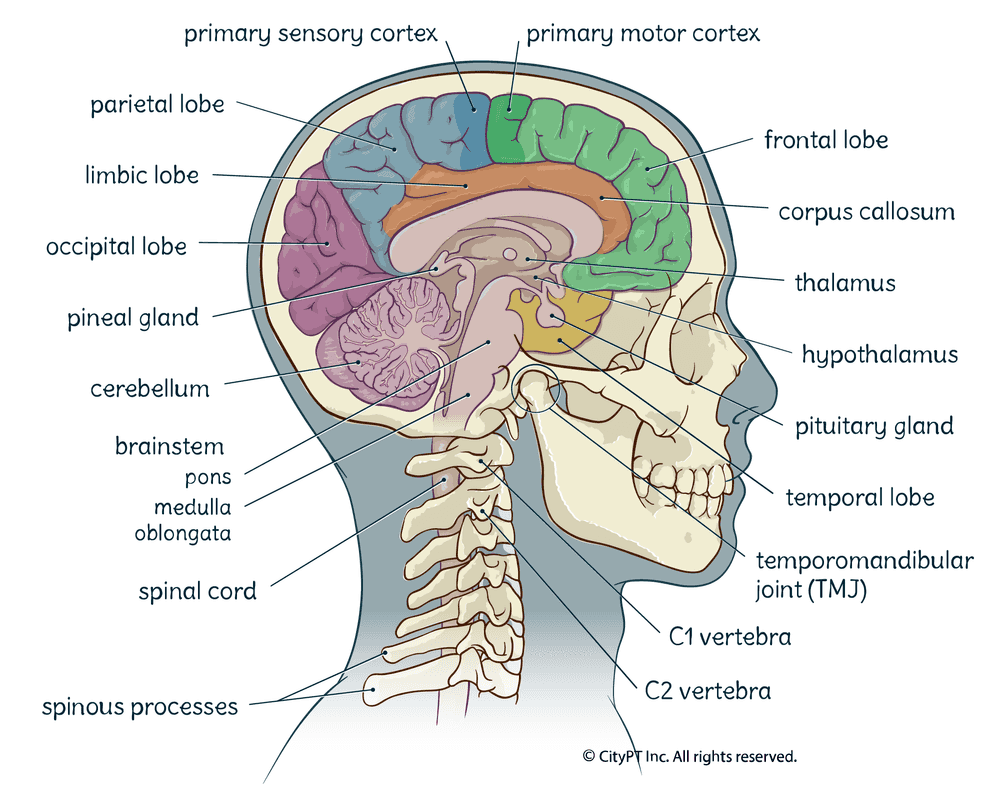
These are just a few of the key areas of the central nervous system that help us function optimally daily! As you can see, when something goes wrong with any part of the brain, it can majorly impact our overall health and well-being — and neurological physical therapy can help address these.
Keeping Brain Tissue Healthy
The entire central nervous system (brain and spinal cord) is supplied with essential nutrients via the bloodstream and a specialized liquid called cerebrospinal fluid (CSF). This fluid surrounds and cushions the brain and removes waste products.
The blood-brain barrier is a special system that helps to protect the brain from harmful substances in the bloodstream. This barrier is made up of cells that tightly fit together and prevent most large molecules and toxins from entering the brain.
Any blockage or injury that affects the bloodstream and CSF can lead to various functional deficits and problems.
Other Important Anatomy of the Head
The bony skull houses and protects the brain, as well as several other important structures, including:
- The eyes
- The ears
- The nose
- The mouth and jaw
- The vestibular system (responsible for balance)
- Muscles of the head that allow us to express ourselves, speak, chew, blink, etc.
In short, the brain and surrounding features are an incredibly complex and important system. And when something goes wrong, whether it's due to a neurological injury or a disease, the effects can be devastating.
What is a Focal Neurological Deficit?
A focal neurological deficit refers to a problem with how one or more specific parts of the brain are working. These deficits are most often visible on imaging results such as magnetic resonance imaging (MRI) and computed tomography (CT scan). This can be caused by damage to the brain, such as from a stroke or head injury, or it can be the result of a neurologic disease like Alzheimer's or Parkinson's. These deficits can cause a wide range of symptoms, depending on which part of the brain is affected, but they are relatively predictable based on which tissues are affected.
Some common focal neurologic signs and altered function include:
- Paralysis on one side of the body, leading to walking problems and other difficulties with daily activities
- Problems with balance and coordination
- Difficulty speaking or understanding speech
- Difficulty reading or writing
- Vision disturbances
- Dizziness
The type, location, and severity of the symptom can indicate which part of the brain or spinal cord is affected and other health conditions being dealt with (comorbidities).3 If you or a loved one are experiencing any of these symptoms, it's important to see a doctor right away. A focal neurological deficit can be a serious condition, and the sudden onset of any symptoms is a medical emergency — the sooner it is diagnosed, the better.
Potential Underlying Causes Include:
- Traumatic brain injury
- Spinal cord injury
- Stroke
- Tumor
- Infection
- Alzheimer's disease
- Parkinson's disease
- Anesthesia
- Medication side effects
We will discuss these further in the section below.
What is a Non-Focal Neurological Deficit?
A non-focal neurological deficit (NFD) refers to a problem with how the brain functions as a whole and is harder to pinpoint. This can be caused by loss of consciousness, emotional issues, or a transient ischemic attack (mini-stroke). These symptoms are more generalized rather than specific neurological signs.
Some common symptoms include:
- Fatigue
- Headaches
- Dizziness
- Depression
- Anxiety
- Altered consciousness
- Feeling generally unwell
Common Causes of Brain Dysfunction
Many other types of abnormal function can occur in the brain — temporary or permanent. These include the following injuries and neurological diseases:
Traumatic Brain Injury (TBI)
A traumatic brain injury (TBI) is an injury to the head that disrupts the brain's normal function. This altered function can be caused by a fall or impact, a car accident, or a blow to the head. TBI can range from mild (concussion) to severe (coma or vegetative state).
Concussion
Concussions are common with impact sports, falls, and car accidents. These are typically considered a "mild TBI" since the symptoms tend to resolve after a shorter period of rest. However, sustaining more than one concussion can lead to progressive, long-term effects over time.
Stroke
A stroke, or cerebral infarction, is an interruption of blood flow to the brain, most often caused by a clot (an acute ischemic stroke) or bleeding (acute hemorrhagic stroke). Symptoms can be gradual or sudden onset and require the attention of emergency medicine, as it will lead to damage or death of brain tissue without immediate care. Common issues after a stroke include movement, vision, and speech problems. What deficits occur depends on which tissues are affected and can vary widely.
Alzheimer's Disease
Alzheimer's is a degenerative neurological disease that affects memory and cognitive function. Theories for the cause of altered brain function surround genetics, aging, lifestyle factors, and chronic disease that affects blood perfusion of the brain.4
Parkinson's Disease
Parkinson's is a degenerative neurological disease that affects movement and coordination. It is caused by the death of neurons in the brain that produce dopamine. The exact reason for why this occurs is unknown, but theories include genetics, environmental factors, and viral infections.5
Anesthesia
Anesthesia is administered for surgery and can have short and long-term effects on the brain. This most often involves changes in cognition. The exact mechanisms are not well understood, but it is thought that anesthesia affects the neurotransmitters (hormones) in the brain.
Medication Side Effects
Some medications can cause brain fog, confusion, and other problems. Examples include:
- Anticholinergics (used for urinary incontinence, allergies, and colds)
- Benzodiazepines (used for anxiety, seizures, and insomnia)
- Statins (used for cholesterol)
- Sleep aids
Check the labels of any medications you are taking to see if brain fog is a potential side effect and talk to your doctor about any concerns.
Multiple Sclerosis (MS)
Multiple Sclerosis is a neurologic disease that attacks the protective layers of neural tissue, causing a wide range of problems. Symptoms may include changes in vision, inability to use the arms or legs (paralysis), and poor balance.6
Heavy Metal Toxicity
Exposure to heavy metals like lead or mercury can cause brain damage. This can lead to symptoms of fatigue, brain fog, headaches, mood changes, achiness, and more.7
Drug Abuse
Recreational drugs like marijuana, cocaine, and heroin can cause brain damage.
Chronic Disease
Chronic diseases like human immunodeficiency virus, diabetes, kidney disease, and liver disease can cause brain damage due to problems with blood flow or inflammation.
Functional Neurological Disorder (FND)
A functional neurological disorder, previously called conversion disorder, is a condition in which psychological stress is converted into physical symptoms. These can include neurological symptoms, paralysis, seizures, blindness, or deafness. The exact cause is unknown, but it is thought to be a combination of genetics and environment.8
These are just a few examples, but many other causes of spinal cord and brain dysfunction exist. If you or a loved one is experiencing any problems with thinking, memory, movement, or mood, it's important to see a physician and neurological physical therapist. Abnormal function of the brain can be a serious condition, and the sooner it is diagnosed, the better.
Other Head Dysfunction
Outside the delicate brain and neural tissues, abnormal function can occur in the head, affecting your daily life. These include:
Headaches
Migraine headaches, cluster headaches, and tension headaches are all types of head pain. While its cause can be related to the brain, it's often associated with nerves and blood vessels in your skull or injury/imbalance of the head and neck muscles. It can also be caused by stiffness (poor mobility) at the base of the skill where it connects to the neck or nerve involvement, such as the occipital or trigeminal nerve.
Temporomandibular Disorder (TMJ) Pain and Dysfunction
Temporomandibular Disorder (TMJ) affects the muscles and joints that connect your lower jaw to your skull. This joint sits in front of your ear. It can cause pain in or around your jaw, ear, face, neck, and head. This can affect your ability to eat, speak, and beyond.
Dental Problems
Tooth decay, gum disease, and other dental problems can cause pain and altered function in your head and face.
Vestibular Dysfunction
This is a problem with the inner ear that can cause dizziness, vertigo, and balance problems. These can be very debilitating, disorienting, and increase the risk of falls as well. One of the most common causes of vertigo is benign paroxysmal positional vertigo (BPPV), where calcium crystals in the ear become dislodged from their normal position in the inner ear canals. This leads to mismatched signals between the brain and eyes, causing an abnormal sensation of movement and, often, nausea.
Hearing Loss
Loud noise exposure, normal aging, and disease can cause this. Hearing loss can make it hard to communicate and understand others.
Tinnitus
Tinnitus is a ringing in the ears that many things, including loud noise exposure, normal aging, and disease, can cause.
Vision changes
Many things, including normal aging, disease, and injury, can cause vision changes. These changes can make it hard to see clearly for daily activities like driving and reading.
These are just a few examples of head dysfunctions that don't specifically involve the brain. These problems can be caused by various factors, including injury, genetics, stress, and overall lifestyle (such as diet). If you are experiencing any type of head pain, it's important to see a doctor to rule out other causes.
How a Neurological Physical Therapist Can Help
Regardless of the underlying cause of your symptoms, there is a very big chance that you are dealing with functional deficits that a physical therapist can help you optimally manage (joint pain, dizziness, imbalance, trouble with movement, reduced quality of life, etc).
Depending on what stage of recovery you are in (and the severity of your health-related issue) you may encounter a physical therapist in the hospital, a rehab center, at home, in a clinical practice, or over a virtual video appointment.
According to the American Physical Therapy Association, there are more than 3,000 board-certified Neurological Clinical Specialists in the U.S. — making it likely there is a provider nearby.
Integrative Medicine for Your Brain and Daily Function
The best way to approach neurological deficits and related spinal cord and brain dysfunction is with an integrative medical team. This means that a team of experts works with you to ensure that you are optimizing your brain health. Examples of medical professionals you may work with include:
- Physical therapist
- Occupational therapist
- Neurologist
- Neuropsychologist
- Speech and language pathologist
- Psychiatrist/Psychologist
Your team will help you determine the underlying causes of your symptoms with differential diagnosis, functional tests, imaging (such as magnetic resonance imaging), neurological screening, and more, to get you the answers you're seeking.
What to Expect from Your Physical Therapist
When working with a neurological physical therapist, you can expect a thorough neurological examination and personalized treatment program to target specific deficits in your nervous system.
The Neurological Physical Therapy Evaluation
The first step is the neurological physical therapy evaluation. The initial evaluation is where your physical therapist will:
- Take a thorough medical history
- Ask you about your lifestyle and general concerns
- Perform a movement analysis
- Assess your balance and coordination (essential functions of the nervous system)
- Test your strength, flexibility, and range of motion
- And more!
This information helps your physical therapist to get an idea of what's going on to help develop an appropriate and effective treatment plan.
Neurological Physical Therapy Treatment
A physical therapist will focus on:
- Improving your strength (motor control), balance, coordination, flexibility, and endurance with guided and at home exercises.
- Teaching you how to properly move your body to minimize pain (known as neuromuscular re-education), use an assistive device with certain activities (if needed),and prevent further injury.
- Enhancing overall physical function (health of the nervous system) and fitness.
- Most importantly, a physical therapist will provide you with extensive education for your specific needs to understand your condition and how to proactively (and effectively) manage it.
You can think of your physical therapist as your partner in problem-solving any difficulties that come your way when recovering from a head, spinal cord, or brain-related injury. Physical therapists can also help you maximize physical function and fitness based on your diagnosis or neurological condition.
Additionally, your physical therapist can make recommendations and referrals for maximizing a healthy lifestyle and reducing the risk of other health problems. This might include finding a dietician, a personal trainer for continued exercise and weight loss (if needed), a mental health care provider, and beyond.
Is Virtual Physical Therapy Appropriate for a Head, Spinal Cord, or Brain Injury?
Yes! In many cases, virtual physical therapy is just as effective (if not more so) than in-person neurological physical therapy. Your physical therapist will be able to assess your situation and give you their professional recommendation on whether virtual or in-person care is best for you.
If you are dealing with any type of head or brain injury, such as a concussion, what type of physical therapy care is best for you will ultimately depend on the severity of your injury, what symptoms you are dealing with, your access to care, and more.
Virtual care for neurological physical therapy has many potential benefits for providing personalized online health information and care for a long-term or chronic neurological deficit or less severe issues like headaches and vertigo9. You can read all about the effectiveness of virtual therapy in our full article.
How to Optimize Your Brain and Spinal Cord Health
Whether you want to reduce your risk of brain-related issues or prevent them from getting worse, keep these tips for maximizing your brain health in mind. You can talk to your physical therapist, physician, and other integrative team members for personalized recommendations.
- Get regular checkups and screenings with your integrative medical team
- Stay active and exercise regularly
- Eat a healthy diet full of brain-boosting nutrients, such as nutrient-dense fruits and vegetables and healthy fats
- Get enough high-quality sleep every night
- Manage stress with relaxation techniques like yoga, meditation, and deep breathing exercises
- Quit smoking and avoid excessive alcohol consumption
- Keep your mind active with daily tasks like reading, puzzles, and learning new things
- Protect your brain during high-impact activities like contact sports (with proper safety gear and training)
- Always wear a seatbelt in your car to reduce the risk of head injury in the event of a crash
- Manage any chronic conditions, such as heart disease and diabetes
Getting the Care You Need: Is It Time?
If you or a loved one are dealing with any type of neurological deficits, whether it's from a head injury, stroke, degenerative disease, or anything else related to the central nervous system, don't hesitate to seek out care. An integrative medical team, including physical therapy, can help you determine the root cause of your symptoms and develop an appropriate treatment plan.
While neurological physical therapy is just one part of the puzzle, it is an integral piece that can help you regain function, improve your quality of life, and reach your goals.
If you're ready to get started on your physical therapy journey to recovery, you can book your first appointment today. Dealing with dysfunction of the brain and head can feel scary. But it doesn't have to be- we'll be with you every step of the way!
This guide is intended for informational purposes only. We are not providing legal or medical advice and this guide does not create a provider-patient relationship. Do not rely upon this physical therapy guide (or any guide) for medical information. Always seek the help of a qualified medical professional who has assessed you and understands your condition.
References
Footnotes
-
Cherry, Kendra. What is Neuroplasticity? Very Well Mind. Updated February 18, 2022. Accessed May 26, 2022. https://www.verywellmind.com/what-is-brain-plasticity-2794886 ↩
-
John Hopkins Medicine. Brain Anatomy and How the Brain Works. Hopkinsmedicine.org. Accessed May 26, 2022. https://www.hopkinsmedicine.org/health/conditions-and-diseases/anatomy-of-the-brain ↩
-
Medline Plus. Focal neurological deficits. National Library of Medicine. Accessed May 26, 2022. https://medlineplus.gov/ency/article/003191.htm ↩
-
National Institute on Aging. What Causes Alzheimer's Disease? Accessed May 27, 2022. https://www.nia.nih.gov/health/what-causes-alzheimers-disease ↩
-
Parkinson's Foundation. Causes. Parkinson.org. Accessed May 27, 2022. https://www.parkinson.org/Understanding-Parkinsons/Causes ↩
-
NHS. Overview- Multiple Sclerosis. Accessed May 27, 2022. https://www.nhs.uk/conditions/multiple-sclerosis/ ↩
-
Ruscio, Michael. Are You Experiencing Heavy Metal Toxicity Poisoning? Dr. Ruscio Blog. Published December 17, 2021. Accessed May 27, 2022. https://drruscio.com/heavy-metal-toxicity-symptoms/ ↩
-
Mayo Clinic. Functional Neurological Disorder. Mayoclinic.com. Accessed May 27, 2022. https://www.mayoclinic.org/diseases-conditions/conversion-disorder/symptoms-causes/syc-20355197 ↩
-
LP. Virtual Reality Vestibular Rehabilitation in 20 Patients with Vertigo Due to Peripheral Vestibular Dysfunction. Med Sci Monit. 2020;26:e930182. Published 2020 Dec 31. doi:10.12659/MSM.930182 ↩
