Simple tasks like tying your shoes or making a meal can become overwhelming when your hand hurts. Grasping and gripping may cause your finger to click, or worse, "lock" down into your palm, especially after waking up in the morning. If this is happening to you, you might have a trigger finger.
Your lifetime risk of developing trigger finger is 2.6%, which jumps to 10% if you have diabetes.1
With trigger finger, gripping or grasping can become so painful you have to stop the daily activities that are most meaningful to you. Luckily, with proper care and guidance, including occupational or physical therapy, you can heal your trigger finger quickly without surgery.2
This guide will give you a quick breakdown of trigger finger, its treatment, and how seeing a Certified Hand Therapist and occupational or physical therapist can help.
Table of Contents
- Understanding Trigger Finger
- Symptoms of Trigger Finger
- What are the Most Common Causes of Trigger Finger?
- Diagnosing Trigger Finger
- What to Expect from Hand Therapy
- Preventing Trigger Finger
- Is It Time to Seek Treatment?
Understanding Trigger Finger
Trigger finger, also called stenosing tenosynovitis, occurs when a finger tendon (that controls the movement of that finger) can't glide smoothly in the tendon sheath around it.
Mild trigger finger may start as a click or dull ache on the palm of your hand. It may progress to causing your affected finger to "lock" into a bent position when gripping or in your sleep — making it hard to keep your finger straight. This is usually very painful, and someone experiencing trigger finger often has to use their other hand to lift their "locked" finger out of their palm.
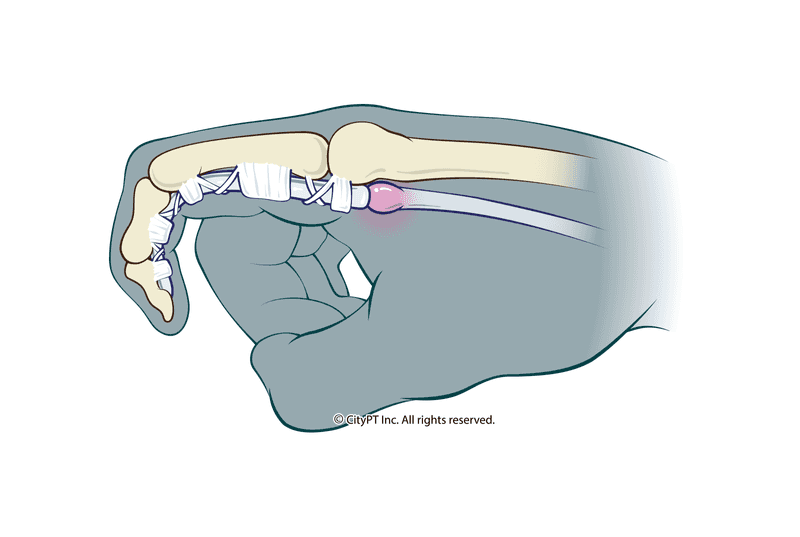
Your hand is a series of strings (tendons) with anchor points (pulleys) to make your tendons more efficient when making a tight fist. You can think of it like a fishing pole with a fishing line.
With trigger finger, your fishing line (tendon) gets a knot from trauma or overuse. When it has to travel on one side or the other of the pulley, the irritation and inflammation are perpetuated, thus increasing the size of the knot and making it progressively harder to move within its own connective tissue (the tendon sheath). This vicious cycle will worsen without proper treatment.
Of note, you can develop trigger finger in any of your digits, including the thumb, called trigger thumb. This often can be due to overuse of the affected thumb tendon from texting and is known commonly as "texting thumb."
Symptoms of Trigger Finger
What are the symptoms of trigger finger? Let's review.
- A dull ache in the palm of the hand
- Progresses to a catching sensation, clicking, or locking of the finger into the palm
- A stuck finger in a bent position (flexed), especially upon waking from sleep
- Difficulty straightening or extending your affected finger
- Decreased ability to perform daily tasks like opening jars, gripping tools, cutting food with a knife
- Tender nodule over your palm just below where your finger meets your palm
- Decreased motion due to pain (especially straightening your finger)
- Swelling in the palm just below where your affected finger meets your palm
What are the Most Common Causes of Trigger Finger?
Trigger fingers are the fourth most common musculoskeletal disorders that result in a referral to a hand specialist, with the thumb and ring finger most affected.1 While less common, it can occur in one or more fingers simultaneously. Below are the most common causes:
- Repetitive stress on the flexor tendons from sustained gripping (as in gardening or hammering)
- Ages 50-70 years old
- Female sex
- More rarely, trauma, like a fall
- Co-morbidities such as diabetes or carpal tunnel syndrome
In addition, certain health conditions increase the risk of developing trigger finger. These include rheumatoid arthritis and diabetes.
Diagnosing Trigger Finger
If you are experiencing palmar hand pain, you can see your primary care doctor, orthopedic surgeon, or local Certified Hand Therapist (CHT), physical or occupational therapist. You should see a CHT for long-term relief and sustainable results to get the best conservative care with less need for pain medications, injections, or surgery.
In other words, a proper diagnosis from a specialist like a CityPT CHT, an occupational or physical therapist with additional specialty training, will help you get better quicker and return to those daily activities that are most meaningful to you, pain-free.
The sooner your hand pain is properly diagnosed, the better the results will be. Therefore, it's best to seek treatment as soon as possible.
What to Expect from Hand Therapy
Waiting to get your painful hand checked out can be scary and overwhelming. Here at CityPT, we strive to make it simple and approachable for you to reduce those anxieties. Let's review what to expect from occupational or physical therapy treatment.
During your first visit, your CityPT therapist will ask questions to get to know you, learn what exactly is troubling you, and understand symptom severity. The questions may be like this:
- How long has your hand pain been bothering you?
- How did it start?
- What makes it better or worse?
- Do you have any medical conditions we should know about?
- What sorts of meaningful daily activities frustrate you because of your hand pain?
- What major life changes have you experienced in the last year?
Your CityPT therapist will also perform a thorough physical evaluation which may include the following:
- Testing to rule out other common conditions
- Measuring range of motion and strength
- Testing functional use of your hand(s)
- Evaluating sensory changes, like numbness or tingling
- Palpating areas of tenderness or areas with scar tissue
- Observing swelling (edema)
- Assessing what positions of the finger or hand promote pain reduction
Occupational or physical therapy treatment may include:
- Custom splinting (typically with extended fingers) to allow the tendon to heal by stopping it from going through the pulley for a time
- Modalities to reduce pain and inflammation, such as heat, ice, ultrasound therapy, or extracorporeal shock wave therapy (ESWT)
- Manual therapy techniques, including soft tissue mobility and finger joint mobility, to increase your range of motion and decrease swelling and pain
- Trigger finger exercises (strength and stretching exercises) to promote blood flow for healing, reduce the risk of developing a "stuck" bent finger, and promote a normal gliding motion
- Functional activities to help increase your independence with daily activities that are most meaningful to you
- Extensive education about your condition and what you can do at home for active recovery, such as home exercises with rubber bands or gentle massaging
Exercises to Try for Trigger Finger
You'll likely find various exercise options if you research "trigger finger exercises." However, it's best to proceed with caution. When the finger tendon is inflamed, forcing finger mobility can harm the surrounding tissues. Initially, reducing the swelling is most important before attempting any informal exercise.
On the other hand, working with a CHT right away will ensure you getting starting with recovery optimally. They will advise what starting positions are best for resting your hand, when to begin stretching exercises, and when it is appropriate to start hand-strengthening exercises for optimal muscular support.
What If Conservative Treatment Doesn't Work?
If caught early, trigger finger has a high success rate with traditional conservative treatment, including occupational and physical therapy. Occasionally, conservative management does not work if you have been experiencing trigger finger symptoms for a long time. If you have tried conservative management and continue to experience persistent pain with no functional improvement, your therapist may refer you to your physician, who may offer additional medical treatment:
- Injections: Corticosteroid injections, while not consistently effective, can offer temporary relief from the pain to allow your body to heal itself. They can be a great adjunct to splinting, manual therapy, and exercise.
- Surgery: When all else has failed, your physician may offer surgical treatment, such as a release of the tendon sheaths to allow your tendon tissue to heal without the irritation from the pulley. You will likely be referred to therapy post-operatively to ease you back into meaningful daily activities. Your hand therapist will help by addressing range of motion, functional adaptations, tendon gliding, swelling and scar management, and increased strength.
Preventing Trigger Finger
Your hand pain may be recent, or you have a job that requires repetitive motion. Do you want to know how to prevent trigger finger from developing or getting worse? Here are some suggestions from CityPT:
- Stay active: An overall active lifestyle can reduce swelling and inflammation in the body. Good circulation means healthy muscles and tendons and less chance of developing inflammatory processes like trigger finger.
- Prevent micro-traumas: By wearing padded gloves (like padded workout gloves) during activities, you can protect the palm of your hand from repetitive stress during tasks like hammering or tool use during gardening.
- Make healthy lifestyle choices: Nutrition can go a long way in the health of your muscles and tendons. Eating nutrient-dense foods and staying hydrated help prevent inflammation in your body. Fortunately, CityPT can get your nutrition on track with one of our Registered Dietitian Nutritionists.
- Try splinting: Over-the-counter trigger finger splints can be helpful in mild cases of trigger fingers. You can often find trigger finger splints online to order.
- Talk to a Certified Hand Therapist: If you have concerns or want professional advice on custom splinting, treatments at home, and functional adaptations, make an appointment with a CityPT CHT.
Is It Time to Seek Treatment?
Perhaps you are waking up in the mornings with your finger stuck painfully in your palm, or maybe you have already tried at-home remedies for your trigger finger without relief. If this sounds like you, it may be time to seek professional help. A CityPT Certified Hand Therapist can customize your care to get you back to living your best life with minimal interruption.
Schedule an appointment with one of our hand specialists today. They will work with you to find the root of your pain and improve your independence with daily activities, getting you on the path to recovery.
This guide is intended for informational purposes only. We are not providing legal or medical advice and this guide does not create a provider-patient relationship. Do not rely upon this guide (or any guide) for medical information. Always seek the help of a qualified medical professional who has assessed you and understands your condition.
References
Footnotes
-
Jeanmonod R, Harberger S, Waseem M. Trigger Finger. [Updated 2022 Jul 20]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2022 Jan-. Available from: https://www.ncbi.nlm.nih.gov/books/NBK459310/ ↩ ↩2
-
Makkouk AH, Oetgen ME, Swigart CR, Dodds SD. Trigger finger: Etiology, evaluation, and treatment. Current reviews in musculoskeletal medicine. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC2684207/. Published June 2008. Accessed August 18, 2022. ↩