Suffering from pain and how to deal with it is certainly a complex issue. Unfortunately, pain has a lot of stigma associated with it in a culture that says things like "brush it off," "no pain no gain," and "it's all in your head."
CityPT was founded to help those suffering from functional impairments and pain-related issues to feel empowered and get the recovery they deserve. To help us understand how people are dealing with pain and what their go-to treatments include, we decided to conduct a small survey to gain some valuable insight into potential barriers to pain management.
Our survey used the SurveyMonkey platform to query roughly 100 participants on whether they had experienced pain that affected their quality of life in the past year, if they sought treatment (particularly physical therapy), and whether they got any relief. We will dive into the results and full discussion below to help guide both clients and clinicians in optimal pain management strategies.
Key Survey Findings
- The vast majority of people that experience debilitating muscle and joint pain do seek help, but their first line of care is internet research and their primary care doctor.
- The main reasons why people did not seek physical therapy were either that they didn't have the time to get a referral from their doctor, or their doctor didn't refer them to PT.
- While 80% of participants sought treatment, those that didn't cited their busy schedule or the hassle of making an appointment as limiting factors. Many also believed their condition would eventually go away.
Table of Contents
- Survey Overview
- Question 1: Screening
- Question 2: Did you seek help for your pain?
- Question 3: Why did you NOT seek help for your pain?
- Question 4: What kinds of help did you seek?
- Question 5: If you DID NOT seek physical therapy, why not?
- Question 6: If you DID seek physical therapy, did it alleviate your pain?
- Question 7 to 12: Demographics
- Conclusion
Survey Overview
A 12-question survey was conducted in the United States in April of 2021 to look at how individuals perceive and deal with pain-related issues. This survey gave insight into how pain treatment was sought, what type of treatment was sought, and what barriers were present to getting treatment.
Since this survey was taken in the midst of the Covid pandemic, it also provides unique insight into how treatment for pain was addressed when social distancing and quarantine were a reality. As society continues it's radical shift towards digital communications, knowing how to approach medical care is key for providing high-quality care in the future.
A total of 113 participants completed this survey from across the U.S. The results provided some valuable insight for consumers and providers alike that we will explore and discuss as we dive into each survey question below.
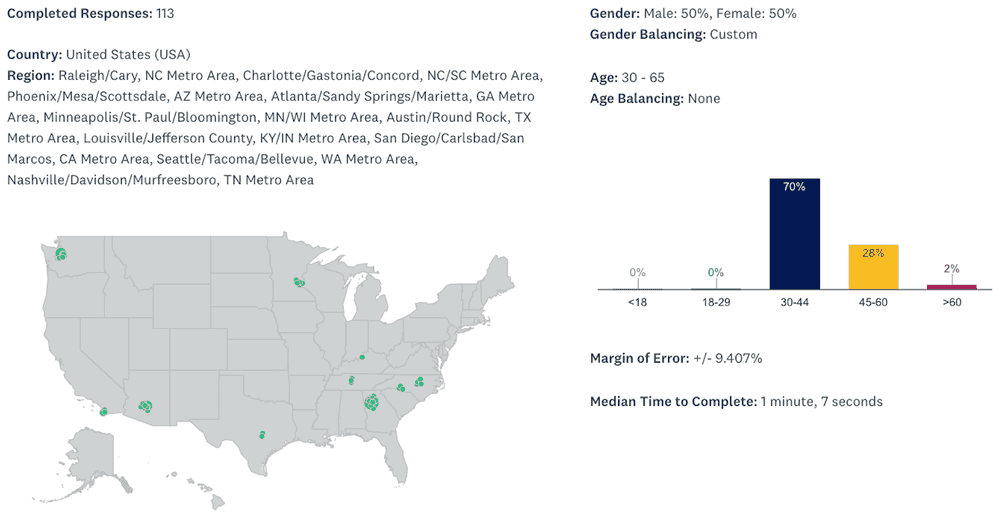
Who took the survey?
Let's take a quick look at the demographics of this survey to gain better awareness of how to interpret the results. Here are the details:
- Number of responses: 113
- Geographic location: United States
- Age Range: 30-65. With the largest group being 30-39 at 51%
- Gender: 50% females, 50% males
Question 1: Screening
The first question was designed as a screen to determine whether the participant would continue with additional questions. If they answered no, the survey was complete. If they answer yes, they continued further:
In the last year, did you have any kind of muscle or joint pain (e.g. lower back pain), that led you to miss work or meaningful activities in your life?
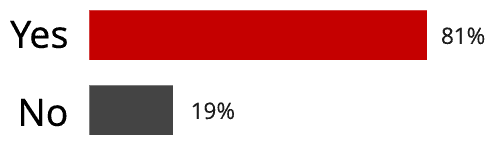
The Result: 80% of people experienced debilitating muscle or joint pain.
We all experience pain sometimes, whether we lift something too heavy, sleep funny, or deal with chronic issues from a past injury. What is most concerning about pain is when it affects our normal daily routine and overall quality of life. When pain is debilitating, it can lead to lost productivity, changes in mental health, canceled events, and less time spend doing what we love.
Common Pain Complaints That Significantly Impact Our Lives
- Low back pain
- Arthritic joint pain (knees, hips, shoulders, ankles, etc.)
- Headaches
- Neurological pain (nerve damage)
- Pain-related disorders, such as fibromyalgia
- Neurological disorders, such as multiple sclerosis
- Pelvic pain associated with a monthly cycle
Why It Matters
Knowing that such a large percentage of the population will deal with pain at some point in their lives demonstrates an immense need for optimizing care and recovery. Helping consumers understand what treatments are available will allow them to get back to work, hobbies, and life with less downtime and suffering.
Ideally, pain is managed acutely to prevent the onset of chronic pain. Chronic pain can lead to disability, poor mental health, and many other negative issues that are best to avoid using proper initial injury treatment.
We will dive into this topic further and what the literature recommends for providing patient-centered care and pain management.
Question 2: Did you seek help for your pain?
The second question was meant to identify individuals that took action beyond their medicine cabinet:
Did you seek help for your pain, other than over-the-counter medications (e.g. Tylenol or Advil)?
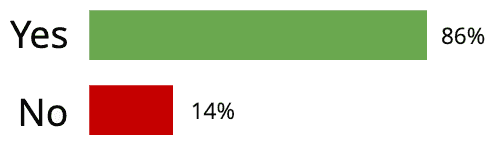
The Result: 86% of participants sought help for their pain.
When pain occurs, intuitively we know that there is something wrong that needs to be addressed. Thus, it's no surprise that the majority of people do take some course of action. We will discuss what these treatments were below, under Question 4.
Getting the Right Care When Pain is Present: Crucial to Save Time, Money, and Unnecessary Suffering
It's great to see that most people recognize professional help can help them manage their pain. This can potentially help them recover quicker, prevent the onset of a chronic condition or re-injury, and move them toward simply feeling their best. However, do consumers truly know what their options are for seeking care? The results of this survey show: maybe, maybe not.
Question 3: Why did you NOT seek help for your pain?
The third question was only asked of those participants that answered NO to Question 2, which was a small sample size of only 16 participants. Participants were allowed to choose multiple answers:
Why did you NOT seek help for your pain?
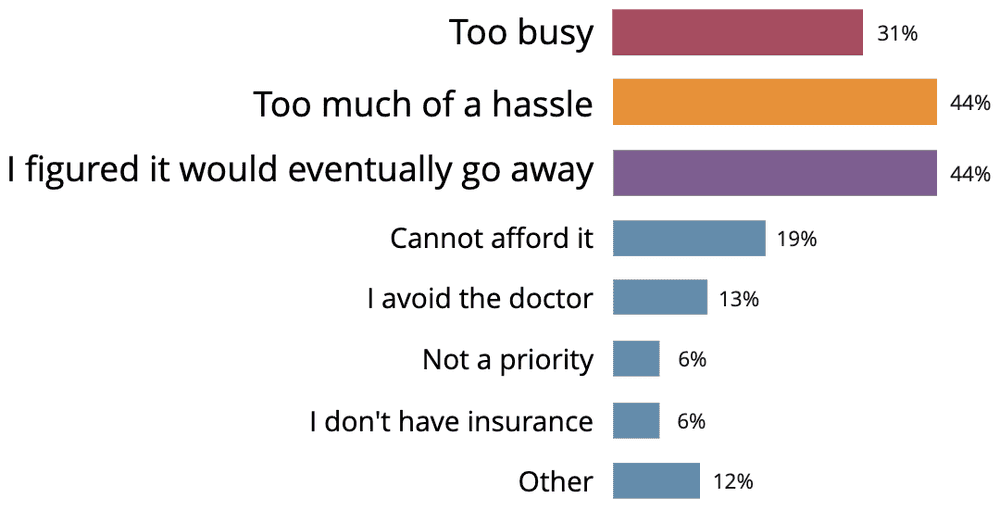
The Result: In summary, participants found it too inconvenient or not necessary to seek help.
Of the 14% of participants that didn't seek treatment for their pain, there were a variety of reasons that they decided not to do so. The top reasons cited included the hassle (44%), assuming the pain would go away over time (44%) and being too busy (31%). Small percentages of people also cited not having insurance, not being able to afford treatment, or simply choosing to avoid the doctor.
Limiting Beliefs Related to Treatment
When something is perceived as being too much of a hassle, it's usually because the potential treatment options are not well understood. Thus, the idea of having to research and figure out how to proceed can feel overwhelming to consumers. This can make it seem easier to do nothing. Yet, the reality is that we could all potentially benefit from personalized professional help.
Additionally, we all tend to live rather busy lives. When we decide something isn't worth our time, it essentially translates to it not being a priority among other competing priorities in our life. Busy professionals, parents, and those dealing with chronic pain or mental health issues may fail to see the potential value in seeking care for their pain troubles.
Will Pain Go Away On Its Own?
Some pain does go away on its own, particularly when it's mild and tied to an event, like stubbing your toe. If the injured area is protected and allowed to heal, pain can certainly resolve on its own. With each passing day or week, the pain may gradually dissipate and full function may return.
Unfortunately, this isn't always the case. Acute pain can get worse or linger and turn into chronic pain, a sign that the body's pain signals have gone awry. Plus, even if the pain does go away on its own, what if the injury keeps occurring due to a lack of awareness of what's triggered the pain in the first place?
Will the Pain Come Back?
Particularly with injuries related to overuse or gradual onset, something triggered the onset of pain. Often this type of pain will return as flare-ups sporadically over the years. These flares could become more intense or more frequent. When the pain becomes disruptive is when an individual might finally seek care. However, a better strategy is to address lingering pain proactively with professional help from a Physical Therapist.
Question 4: What kinds of help did you seek?
The fourth question, asked only if the participant answered yes to Question #2, was designed to elicit what participants perceive as their go-to sources of pain relief. Participants were allowed to choose multiple answers:
What kinds of help did you seek?
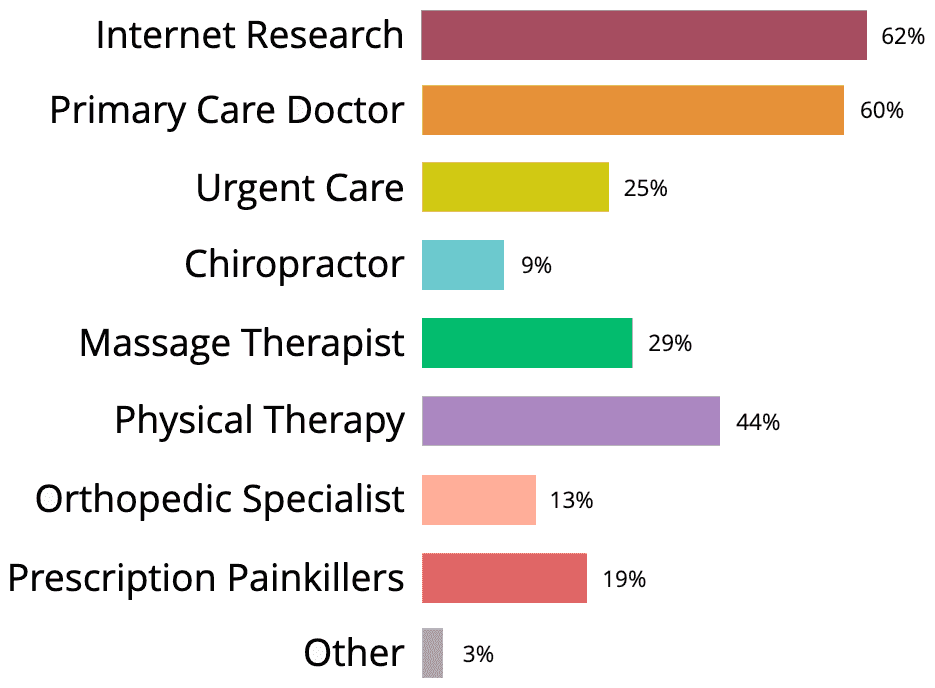
The Result: Survey participants clearly perceive the internet and their primary care doctor as the first line of defense against musculoskeletal pain.
Does the Internet Have All the Answers?
With access to the world wide web, it's easier than ever to find the "answer" to any problem. Of course, the internet is filled with recommendations that yield confusing, conflicting, and ambiguous advice. Additionally, the answers are inherently generic to appeal and apply to the general population. It would be interesting to know how many of these queries actually yielded positive and helpful results.
What Does a PCP Do for Pain?
The large majority of people go to their primary care doctor when they experience pain. In fact, back pain (defined as the low back or neck) is one of the top 10 reasons that patients visit their physician.1 Unfortunately, treatments and recommendations for back pain can vary significantly between PCPs, depending on factors like geographical location and type of pain (acute vs. chronic).2
While a non-pharmacological approach was reported as the preferred initial treatment, there is still a large number of PCPs that prescribe pain medication as one of their first lines of defense against pain. More research is needed to better understand the reason for this since study after study demonstrates the efficacy of physical therapy interventions as alternatives to pills, and physicians have an obligation to utilize validated research in their clinical decision making processes.
Unfortunately, the instinct that patients have to immediately turn to their PCP for help with musculoskeletal pain can be traced back to the directives of insurance companies, which leaves the onus on the healthcare consumer to discover on their own that this is not always the best decision.
Question 5: If you DID NOT seek physical therapy, why not?
The fifth question was used better understand why most patients don't routinely seek physical therapy for their muscle and joint pain:
If you DID NOT seek physical therapy, why not?
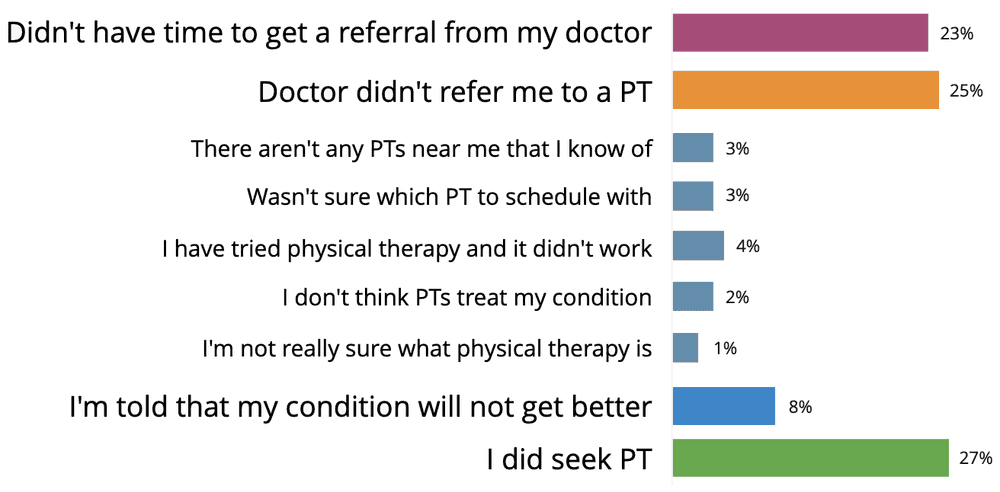
The Result: Here again, we find that inconvenience keeps people from seeking the care they need. And we also see that even if someone overcomes the inconvenience, there's a high likelihood their doctor won't refer them to physical therapy.
Doctor Referrals and PT: Are They Necessary?
This question was perhaps the most revealing one from this survey. It illustrates the lack of knowledge regarding what is necessary to see a physical therapist. In this case, almost one in four people didn't realize they could go directly to a physical therapist for care without a referral. Or, they didn't realize that a physical therapist is a specialist in the very thing that was troubling them, not their PCP.
Direct access has been around in all 50 states since 2015 on some level. There may be limitations due to insurance, however. For example, some states require a referral for certain treatments. And, Medicare is the only insurance that requires a referral from a primary care physician to see a PT.
Many people don't realize that a skilled physical therapist can address psychosocial issues, screen for red flags, refer out as needed, and administer non-pharmacological care. It's why many high-quality studies have illustrated the potential benefits of seeking care from a physical therapist first3. In fact, getting PT first yielded less downtime, less dependence on opioids, and a reduced risk of needing invasive surgery. This equates to the possibility of immense savings and peace of mind for the recovering patient.
Why Aren't Doctors Referring to PT for Pain Management?
Physical therapy interventions are one of the top non-pharmacological options for treating pain-related issues, such as joint pain, muscle pain, and injuries because of the multifaceted approach it takes.4 So why are 25% of survey participants reporting they didn't get a referral after seeing their doctor for initial pain management?
Just as patients didn't realize that direct access was a possibility, this statistic shows that some primary providers are not aware either. Plus, the doctors may not have personal experience or understand the benefits of physical therapy themselves.
This is where provider education and partnerships can help them understand what specialties are available, the potential benefits of physical therapy, and when it is indicated for their patients that are experiencing pain or other dysfunctions.
Question 6: If you DID seek physical therapy, did it alleviate your pain?
The sixth question was intended to determine how effective participants found their physical therapy:
If you DID seek physical therapy, did it alleviate your pain?
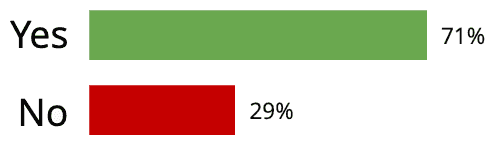
The Result: 71% reported pain relief
The majority of surveyed participants were able to get at least some pain relief from the physical therapy intervention they received. This is good news for anyone suffering from pain that wants to get back to normal life.
Optimal Pain Management Treatment Methods with PT
The most appropriate treatment for a given pain-related issue can vary with each individual. Yet, there are some general guidelines a physical therapist typically follows to yield the best possible result.5
For example, it has been shown that the treatment of acute mechanical (non-sinister) lower back pain responds best to reassurance, extensive education, teaching self-management, and encouraging regular activity.
Chronic low back pain also responds well to the above recommendations, in addition to personalized exercise recommendations and spine manipulation.
The Role of Psychosocial Factors for Effective Pain Management
Perhaps most importantly, the way an individual approaches the onset or continuation of pain can have a large influence on their ability to recover. Anxiety, fear, and a sense of helplessness can contribute to poor healing and the onset of chronic pain.
Addressing these underlying fears to help someone suffering from pain feel empowered and confident in their recovery is arguably the single most important factor to a successful recovery. Clinicians that focus on providing in-depth education and accountability to their patients are more likely to see better outcomes.
Question 7 to 12: Demographics
These questions simply provided insight into the individuals surveyed. They revealed a younger population primarily in their 30s. This illustrates pain isn't just experienced by the elderly, as is often assumed.
In Review: Top Barriers to Pain Management by Utilizing PT
Let's review the top barriers and challenges to treating pain with physical therapy.
- Lack of time
- Perceived as a hassle
- Too busy
- Assuming the pain will dissipate on its own
- Not able to get a referral (or perceiving they needed one)
- Not being referred by their provider
- Choosing to search the internet for answers
- Choosing to go to their PCP first
- A negative past experience with PT
To all the physical therapists reading this: Is there a way we can do better? How do we reach the people that could use our help the most? How do we help them understand the potential benefits they stand to gain?
How to Improve Pain Management Outcomes
Making an impact on better pain management practices and outcomes starts with awareness. As physical therapists, it's important to gain visibility and help potential clients understand the benefits of seeking care. This starts with building trust and authority in the community via conversation, education, and promotion. This survey revealed the potential value of networking with local physicians to gain this visibility.
Additionally, some people may not even realize that they are a candidate for treatment in the first place, while others may have given up and don't think PT will be able to help. Helping them understand what treatments are available and how they can help might give them the nudge they need to get on track with an effective care plan.
As access to PT gets continually easier, the hope is that anyone suffering from pain or injury can get the help they need. Direct access opportunities in each state are a great start to easier access to PT. Plus, the growth of virtual physical therapy holds immense promise for reaching those that cite time and inconvenience as their primary barrier.
Conclusion
Looking to the future, the continued growth of virtual PT might be one possible solution. It will allow easier access, consistent treatments, and better overall satisfaction for pain management. After all, high-quality and effective treatment isn't associated with where a clinic is located or the use of top-of-the-line equipment. Rather, it is associated with continued monitoring, establishing good rapport, and addressing psychosocial factors. Patient-centered care, whether it's face-to-face or virtually, is the key to proper pain management.
As a growing PT platform, CityPT conducted this survey to gain insight into current trends of consumer behavior. We truly believe that many people are missing out on the great potential benefits of PT. Knowing what the barriers to treatment are and how to best address them will pave the way for better pain management options in the future.
Before you go, please read our disclaimer. This blog is intended for informational purposes only. We are not providing legal or medical advice and this blog does not create a provider-patient relationship. Do not rely on our blog (or any blog) for medical information. Always seek the help of a qualified medical professional who has assessed you and understands your condition.
References
Footnotes
-
What are the common conditions in primary care? https://www.ncbi.nlm.nih.gov/pmc/articles/PMC6234945/ ↩
-
Roseen, Eric J.; Conyers, Frank Garrett; Atlas, Steven J.; Mehta, Darshan H. Initial Management of Acute and Chronic Low Back Pain: Responses from Brief Interviews of Primary Care Providers. The Journal of Alternative and Complementary Medicine. Vol/ 27, No. S1. https://www.liebertpub.com/doi/10.1089/acm.2020.0391#:~:text=For%20chronic%20LBP%2C%20most%20PCPs,least%20one%20medication%20(39%25). ↩
-
Frogner, Bianca K. PhD, et al. Physical Therapy as the First Point of Care to Treat Low Back Pain: An Instrumental Variables Approach to Estimate Impact on Opioid Prescription, Health Care Utilization, and Costs. Health Services Research. Volume 53, Issue 6. December 2018. Pages 4629-4646. https://onlinelibrary.wiley.com/doi/abs/10.1111/1475-6773.12984 ↩
-
Lin I, Wiles L, Waller R, et alWhat does best practice care for musculoskeletal pain look like? Eleven consistent recommendations from high-quality clinical practice guidelines: systematic reviewBritish Journal of Sports Medicine 2020;54:79-86. https://bjsm.bmj.com/content/54/2/79 ↩
-
Shipton, Edward E. Physical Therapy Approaches in the Treatment of Low Back Pain. Pain Ther 7, 127–137 (2018). https://link.springer.com/article/10.1007/s40122-018-0105-x#citeas ↩

JayDee Vykoukal is an author, holistic health coach, mom blogger, and passionate Doctor of Physical Therapy. She loves teaching healthy living, writing about motherhood, traveling and spending quality time with her family.

JayDee Vykoukal is an author, holistic health coach, mom blogger, and passionate Doctor of Physical Therapy. She loves teaching healthy living, writing about motherhood, traveling and spending quality time with her family.



